News
UK doctors strike: NHS says hospitals holding up
NHS leadership says hospitals are coping with the UK doctors strike so far, as services adapt, patient safety is prioritised and talks stall.
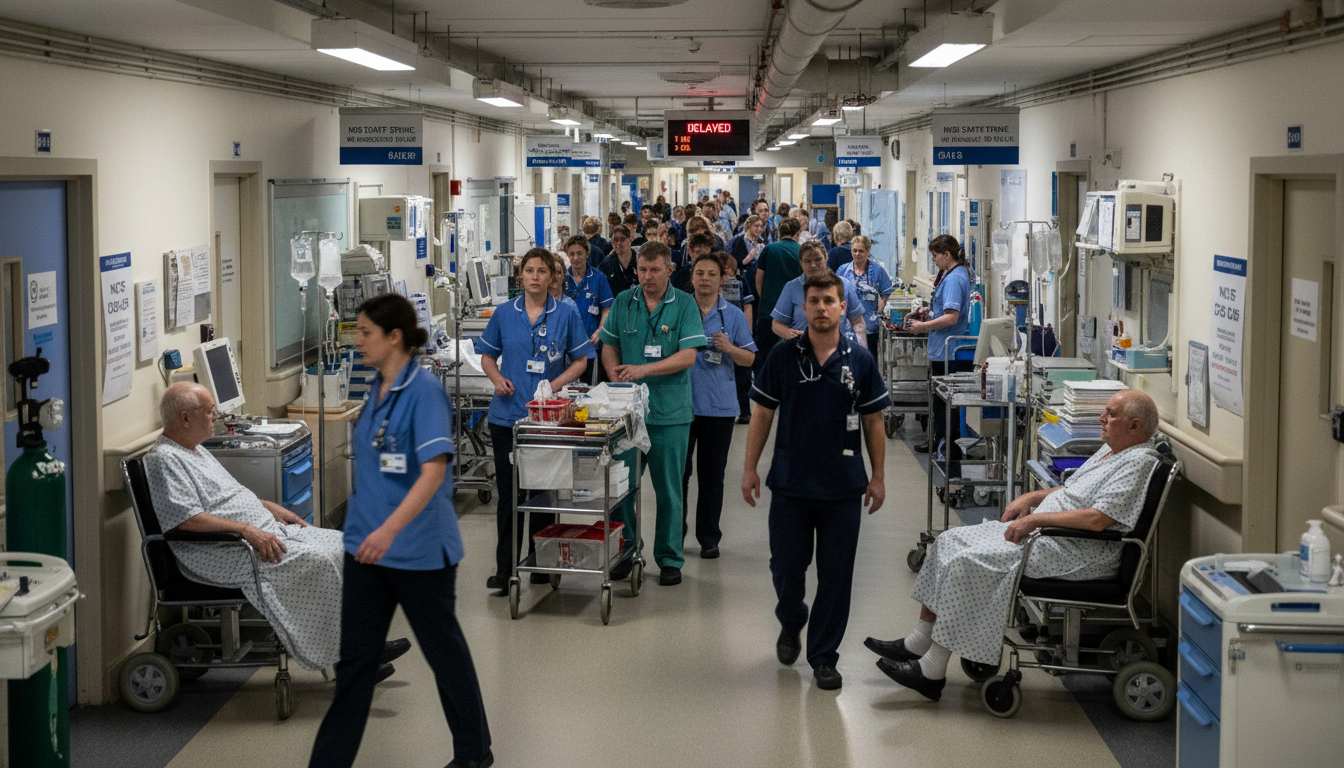
NHS Chief Comments on Hospital Strategy
Senior NHS leadership said hospitals are coping well so far with the UK doctors strike, pointing to pre planned rotas, consultant cover and prioritisation of time critical work. Today, managers across trusts have leaned on escalation plans that were rehearsed ahead of walkouts, keeping emergency departments staffed and ensuring maternity, cancer and critical care pathways remain protected. The message from the centre has been that resilience is built on clear decision making locally, with extra capacity moved to the highest risk wards and theatres, and elective activity pared back where staffing cannot be guaranteed. Leaders also stressed that incident control rooms are tracking pressures across regions and redistributing support when a site shows early signs of strain.
Impact of Strikes on Patient Care
The immediate hospital impact has been seen most clearly in postponed non urgent appointments, as trusts balance safe staffing against the need to keep urgent flows moving. Live site reports have focused on queue management in emergency departments, faster senior review, and tighter discharge coordination to preserve beds for arrivals. In some areas, patient messaging has been sharpened so people understand which services are open and what symptoms require prompt assessment. Those operational updates have echoed the tone of a separate market briefing at Bitcoin Hits a Critical Point in the Market Cycle, in that both rely on rapid monitoring rather than guesswork. NHS strike planning has centred on avoiding unsafe delays, with clinical teams stepping into roles normally filled by juniors.
Background on Pay Dispute
The junior doctors pay dispute remains the central fault line, with clinicians arguing that real terms earnings have eroded over more than a decade and that recruitment and retention are being damaged. Update statements from union representatives have framed the walkout as a last resort after talks failed to produce an offer they consider credible, while ministers have repeatedly cited budget limits and existing pay review processes. Trust leaders have largely avoided taking sides, but many have acknowledged that staffing gaps are already a daily constraint, separate from strike action. In practice, the pay argument shows up on the ward through rota fragility and reliance on temporary cover, which increases costs and makes long term workforce planning harder.
Government and Union Responses
Government messaging has emphasised that emergency care remains available and that patients should continue to use services when needed, while urging the union to return to negotiations. The union has countered that sustained action is necessary to shift the position on junior doctors pay, arguing that service pressures will not ease without a settlement that stabilises the workforce. Today, both sides have used public updates to reinforce their credibility, with officials pointing to contingency measures and the union pointing to turnout and member support. Reporting from major outlets has tracked these lines closely, including coverage at the BBC’s latest reporting on the doctors’ strike. Trusts, caught in the middle, have asked for clarity quickly to reduce disruption.
Future Implications for UK Healthcare
Beyond the current stoppage, the policy risk is that repeated disruption becomes normalised, stretching elective recovery and complicating efforts to cut waiting lists. Live operational stress also feeds into staff morale, because teams asked to cover extra shifts may face fatigue and reduced training time, even when patient safety is maintained. A durable settlement would help restore planning certainty, but it would also set expectations for other groups watching closely. Update implications are already being discussed in terms of how future pay deals are structured and how workforce supply is funded, with an eye on reducing dependency on short term locum spending. For patients, the key test is whether postponed care can be rebooked quickly without creating fresh bottlenecks later in the year.
Alongside workforce negotiations, the NHS is trying to keep public guidance simple, use services appropriately, and avoid people delaying care out of fear that hospitals are closed. Trust communications have reiterated that urgent and emergency pathways are functioning, and that the safest option for worrying symptoms is still to seek medical advice. Operational leaders have also leaned on standard pathways and national information to keep messages consistent, directing people to official resources on NHS.uk patient guidance and service information rather than social media rumours. The overarching aim is to hold a stable line until the strike ends, then restore capacity quickly. If negotiations resume, both sides will be judged on speed, clarity and a willingness to reduce avoidable harm.



















