Latest News
Mother Says NHS Failed Her After Baby Dies Days After Home Birth in London Hospital Case
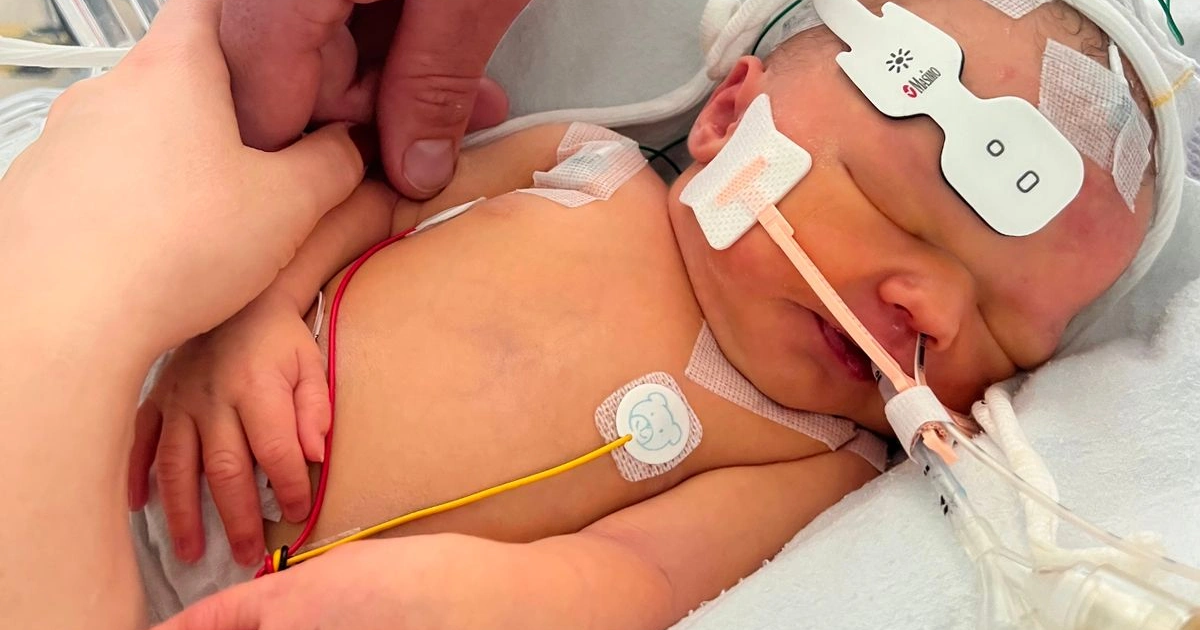
A mother has said she was failed by the NHS following the death of her newborn daughter who died at a central London hospital just one week after a planned home birth. The baby, Poppy Hope Lomas, died at University College Hospital after experiencing severe complications linked to oxygen deprivation around the time of birth. The case has raised serious questions about maternity care, risk assessment, and decision making processes within NHS home birth services, particularly when medical advice and parental wishes may come into conflict.
An inquest into the death heard that the mother, Gemma Lomas, had been supported by a home birth midwifery team linked to Barnet Hospital under the Royal Free London NHS Foundation Trust. The planned home delivery was carried out despite concerns later highlighted during the investigation. It was stated that the birth involved multiple risk factors that were not adequately addressed or escalated before the delivery took place, despite existing clinical guidance advising caution in similar circumstances.
The senior coroner overseeing the inquest concluded that the trust had agreed to proceed with a home birth that was considered unsafe and not in line with established medical guidance from professional obstetric bodies. Evidence presented suggested that there was a failure to properly communicate the level of risk involved to the mother and to ensure that all relevant clinical warnings were fully considered before the decision to proceed with a home birth was made. The findings have added to ongoing scrutiny of maternity services and decision making protocols within NHS trusts.
Medical reports presented during the inquest indicated that Poppy Hope Lomas likely suffered a severe hypoxic ischaemic brain injury shortly before birth, a condition caused by a lack of oxygen reaching the brain. This type of injury is known to be extremely serious and can occur in situations where complications arise during labour. The baby was transferred to hospital following the home birth but died seven days later despite medical intervention, leaving the family devastated by the outcome.
The case has sparked renewed discussion about the balance between promoting natural birth options and ensuring patient safety within maternity care systems. Healthcare professionals and regulators are expected to review the circumstances surrounding the case as part of broader efforts to improve risk assessment procedures and communication between medical teams and expectant mothers. The findings are likely to contribute to ongoing debates about how home birth services are managed and how safety standards are applied in high risk situations.










